Uremia is a serious medical condition that arises when the kidneys are no longer able to effectively remove waste products from the bloodstream. Derived from the Greek words “ouron” (urine) and “haima” (blood), uremia literally means “urine in the blood.” It is not a disease in itself but a complication of chronic kidney disease (CKD) or acute kidney injury (AKI), signaling that kidney function has deteriorated severely.
In this comprehensive guide, we will explore the signs and symptoms of uremia, the causes, diagnosis, complications, and treatment options available. Whether you’re a patient, caregiver, or healthcare professional, understanding uremia can aid in early detection and improve patient outcomes.
What Is Uremia?
Uremia occurs when the kidneys fail to filter nitrogenous waste products, such as urea and creatinine, from the blood. As these toxins accumulate, they disrupt the normal chemical balance of the body, affecting almost every organ system. Left untreated, uremia can lead to multi-organ failure and death.
Causes of Uremia
Uremia is commonly associated with:
Chronic Kidney Disease (CKD): Gradual decline in kidney function over time.
Acute Kidney Injury (AKI): Sudden loss of kidney function, often reversible with prompt treatment.
End-Stage Renal Disease (ESRD): Final stage of chronic kidney disease requiring dialysis or transplantation.
Other contributing factors may include:
Obstructive uropathy (e.g., kidney stones or enlarged prostate)
Use of nephrotoxic drugs
Signs and Symptoms of Uremia
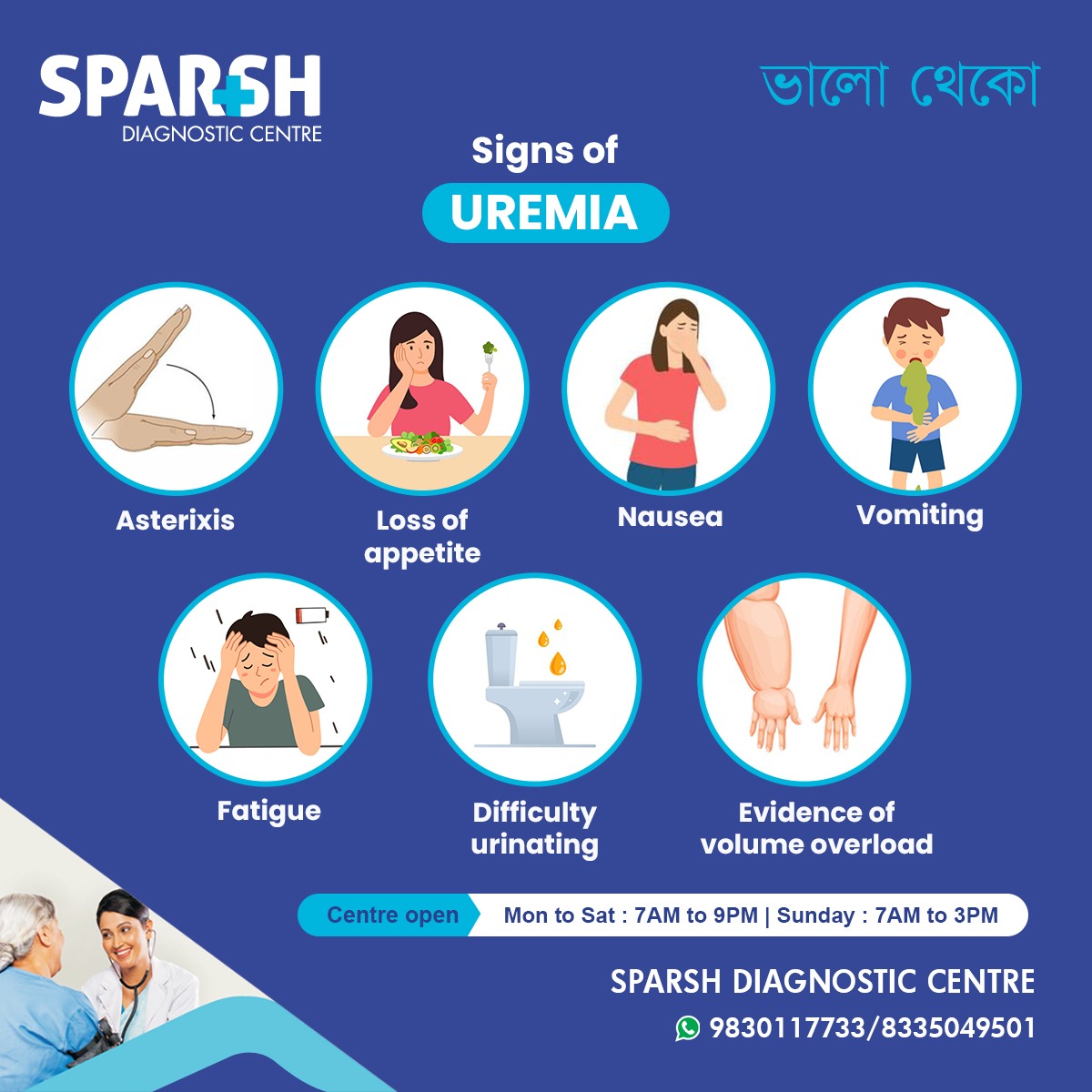
As shown in the Sparsh Diagnostic Centre infographic, uremia presents with a variety of signs and symptoms due to the systemic accumulation of waste products:
1. Asterixis (Flapping Tremor)
Asterixis is a characteristic sign of uremia and indicates encephalopathy. It manifests as a flapping motion of the hands when the arms are extended and wrists bent back. It reflects the brain’s impaired ability to regulate motor function due to toxin buildup.
2. Loss of Appetite
Patients with uremia often experience anorexia. The buildup of waste products in the blood affects the gastrointestinal system, leading to a metallic taste in the mouth, bad breath (uremic fetor), and general disinterest in food.
3. Nausea and Vomiting
Gastrointestinal disturbances are common. Patients may complain of persistent nausea and may vomit due to elevated levels of urea and other toxins irritating the stomach lining.
4. Vomiting
Vomiting may become frequent as uremia progresses. In severe cases, patients may vomit blood due to gastrointestinal ulceration, known as uremic gastritis.
5. Fatigue
Extreme tiredness is a hallmark of uremia. It results from anemia of chronic disease, poor oxygenation, and general metabolic imbalance. Patients often report being unable to perform daily activities.
6. Difficulty Urinating
As kidney function declines, urine output often decreases, leading to oliguria (less than 400 ml of urine/day) or even anuria (complete absence of urine). This indicates severe renal impairment.
7. Evidence of Volume Overload
Swelling in the legs, face, or abdomen (edema) and shortness of breath may occur due to fluid retention. Pulmonary edema, a life-threatening condition, can result if fluid accumulates in the lungs.
Other Symptoms to Watch For
In addition to the signs above, patients may also experience:
Confusion and cognitive changes
Muscle cramps and twitching
Pruritus (severe itching)
Pallor due to anemia
Hypertension
Bleeding tendencies (due to platelet dysfunction)
Pathophysiology: How Uremia Develops
The kidneys serve as filters that excrete nitrogenous waste and regulate fluid, electrolytes, and acid-base balance. When the kidneys fail:
Urea, creatinine, and other waste products accumulate.
Electrolyte imbalances occur (e.g., hyperkalemia, hyponatremia).
Hormonal functions like erythropoietin production are impaired.
Immune and neurological functions are compromised.
Diagnosis of Uremia
A clinical diagnosis of uremia relies on history, physical examination, and diagnostic testing:
Blood Tests
Serum urea nitrogen (BUN): Elevated
Serum creatinine: Elevated
Electrolytes: May reveal hyperkalemia, hyperphosphatemia
eGFR (estimated Glomerular Filtration Rate): Decreased
CBC: Anemia of chronic disease
Urine Tests
Proteinuria
Hematuria
Urine sodium, osmolality
Imaging
Ultrasound of kidneys: May show shrinkage or structural abnormalities
CT/MRI: If obstructive causes or complications are suspected
Other Tests
ECG: To detect hyperkalemia-related cardiac abnormalities
Renal biopsy: May be needed in certain glomerular disorders
Complications of Uremia
Uremia is not just about elevated toxin levels—it can lead to severe complications, such as:
Uremic encephalopathy
Pericarditis
Uremic bleeding (platelet dysfunction)
Infections
Electrolyte imbalances (especially life-threatening hyperkalemia)
Without timely intervention, these complications can be fatal.
Treatment of Uremia
Treatment focuses on addressing the underlying cause, managing symptoms, and removing accumulated toxins:
1. Dialysis
Dialysis is the cornerstone of uremia management in advanced kidney failure:
Hemodialysis: Blood is filtered through a machine.
Peritoneal dialysis: Uses the peritoneal membrane as a filter.
2. Kidney Transplantation
For eligible patients, kidney transplantation offers a long-term cure, restoring normal renal function and eliminating the need for dialysis.
3. Medications
Erythropoietin-stimulating agents: For anemia
Phosphate binders: To manage hyperphosphatemia
Antihypertensives: To control blood pressure
Diuretics: For fluid overload (if residual kidney function exists)
Sodium bicarbonate: For metabolic acidosis
4. Nutritional Support
A renal-friendly diet is essential:
Low protein (in early CKD)
Low potassium and phosphorus
Sodium and fluid restriction
Adequate caloric intake to prevent catabolism
Preventing Uremia
Uremia is often preventable with early intervention and effective management of underlying conditions.
Tips for Prevention:
Control diabetes and hypertension: Leading causes of kidney failure
Avoid nephrotoxic drugs: NSAIDs, certain antibiotics
Stay hydrated: Unless on fluid restriction
Follow up regularly: With a nephrologist if you have kidney issues
Maintain a healthy lifestyle: Diet, exercise, and weight management
When to See a Doctor
Seek immediate medical attention if you experience:
Reduced or no urine output
Swelling in legs or face
Confusion or altered mental status
Shortness of breath
Persistent nausea or vomiting
Early detection can make a crucial difference in managing uremia and preventing complications.
Uremia is a serious, potentially life-threatening condition that signifies advanced kidney failure. Recognizing the warning signs—like asterixis, fatigue, loss of appetite, and difficulty urinating—is key to prompt diagnosis and treatment. With advancements in dialysis and kidney transplantation, many patients can lead fulfilling lives despite kidney failure. However, the emphasis should always be on prevention, early diagnosis, and careful management of risk factors such as diabetes and hypertension.
If you or a loved one are experiencing symptoms of uremia, don’t wait. Consult a nephrologist or visit your nearest diagnostic centre, such as Sparsh Diagnostic Centre, for timely evaluation and care.
Sparsh Diagnostic Centre
📞 Call: 9830117733 / 8335049501
📍 Centre Open:
Mon to Sat: 7 AM – 9 PM
Sunday: 7 AM – 3 PM
Your health is our priority. Stay safe, stay healthy.
#BhaloTheko
Disclaimer:
No content on this site, regardless of date, should ever be used as a substitute for direct medical advice from your doctor or other qualified clinician.

![]()






[…] Severe drowsiness or coma (in cases of severe uremia) […]
[…] Dialysis: if due to uremia […]
[…] Uremia – Buildup of toxins causing confusion, nausea, or coma […]