Respiratory Distress Syndrome (RDS) is a serious medical condition that affects breathing, most commonly seen in premature newborns but also occurring in adults under certain circumstances. While the name may sound technical, the concept is straightforward: the lungs struggle to function properly, making it difficult for the body to get enough oxygen.
If you’re a parent, caregiver, or simply looking to understand this condition better, this guide breaks it down in a clear and practical way—without overwhelming medical jargon.
What is Respiratory Distress Syndrome?
Respiratory Distress Syndrome is a condition where the lungs cannot expand and function effectively due to a lack of a substance called surfactant.
Surfactant is a natural fluid produced in the lungs that keeps the tiny air sacs (alveoli) open. Without it, these air sacs collapse, making breathing extremely difficult.
There are two main types:
- Neonatal RDS (NRDS): Seen in premature babies
- Acute Respiratory Distress Syndrome (ARDS): Seen in older children and adults due to illness or injury
This blog focuses primarily on neonatal RDS, as it is more common and directly linked to lung development.
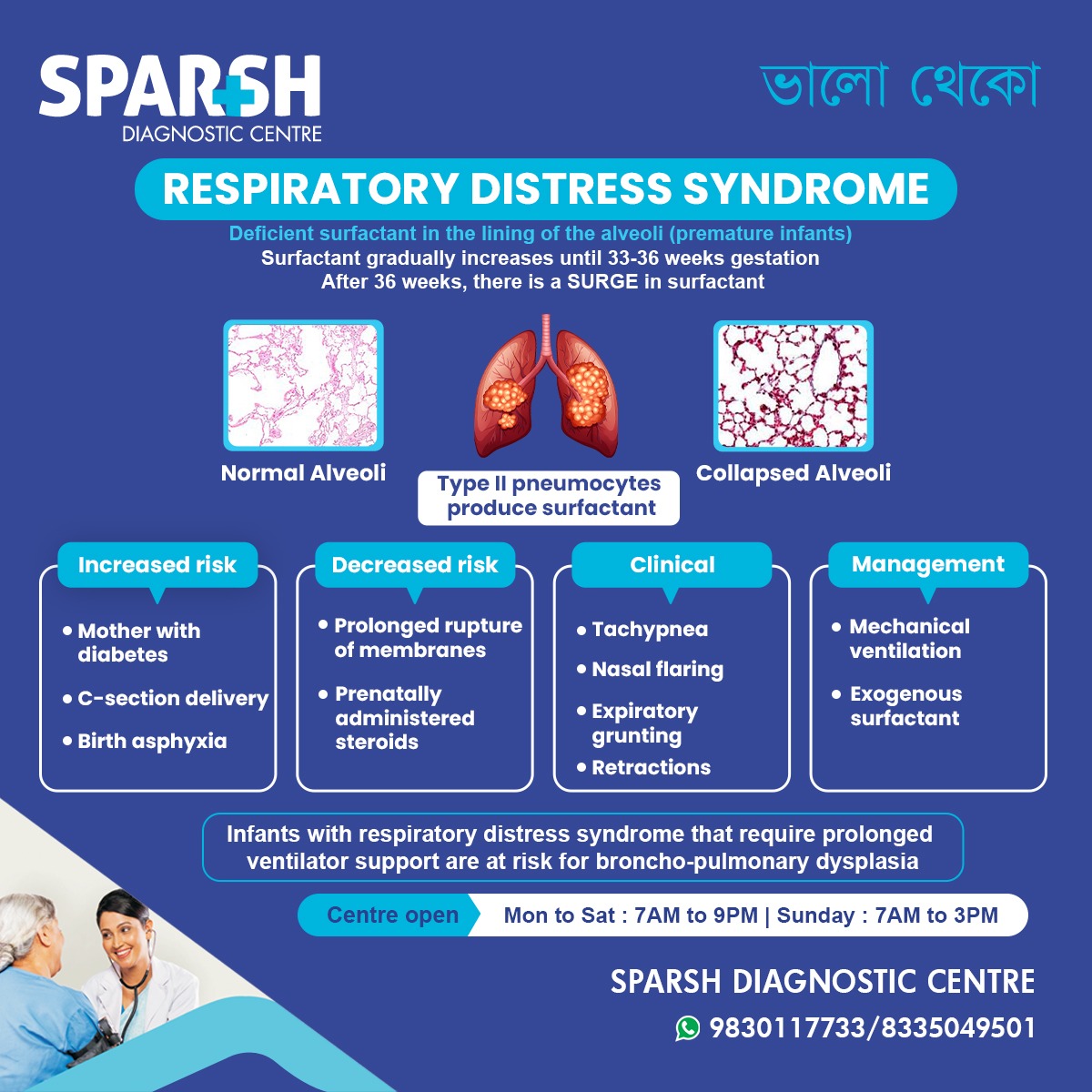
Why Does Respiratory Distress Syndrome Occur?
The primary cause of neonatal RDS is immature lungs.
The Role of Surfactant
In a developing fetus:
- Surfactant production begins around 24–28 weeks of pregnancy
- It increases steadily
- A significant surge occurs after 34–36 weeks
Babies born before this timeline often don’t have enough surfactant, leading to collapsed alveoli and breathing difficulty.
Risk Factors for Respiratory Distress Syndrome
Certain factors increase the likelihood of RDS in newborns.
Increased Risk Factors
- Premature birth (before 37 weeks)
- Mother with diabetes
- Cesarean (C-section) delivery without labor
- Birth asphyxia (lack of oxygen during birth)
- Multiple births (twins, triplets)
- Male gender (slightly higher risk)
Protective (Decreased Risk) Factors
Interestingly, some conditions reduce the risk:
- Prolonged rupture of membranes
- Antenatal steroid therapy
- Stress before birth (which may accelerate lung maturity)
Signs and Symptoms of Respiratory Distress Syndrome
Symptoms of RDS usually appear immediately after birth or within the first few hours.
Common Symptoms
- Rapid breathing (tachypnea)
- Grunting sounds during exhalation
- Nasal flaring
- Chest retractions (skin pulling in between ribs)
- Bluish skin (cyanosis) due to low oxygen levels
These signs indicate that the baby is working hard to breathe and needs urgent medical attention.
How is Respiratory Distress Syndrome Diagnosed?
Doctors rely on a combination of clinical signs and diagnostic tests.
Diagnostic Methods
- Physical examination
- Observing breathing patterns and oxygen levels
- Chest X-ray
- Shows a “ground-glass” appearance typical of RDS
- Blood gas analysis
- Measures oxygen and carbon dioxide levels
- Pulse oximetry
- Monitors oxygen saturation in real time
Early diagnosis is crucial for effective treatment and improved outcomes.
Treatment of Respiratory Distress Syndrome
Treatment focuses on supporting breathing and improving oxygen delivery.
1. Oxygen Therapy
Mild cases may only require supplemental oxygen through:
- Nasal prongs
- Oxygen hood
2. Continuous Positive Airway Pressure (CPAP)
CPAP helps keep the airways open by delivering constant air pressure, preventing alveolar collapse.
3. Mechanical Ventilation
In severe cases, a ventilator is used to assist or take over breathing.
4. Surfactant Replacement Therapy
This is one of the most effective treatments.
- Artificial surfactant is delivered directly into the lungs
- Helps the alveoli stay open
- Significantly improves survival rates
5. Supportive Care
- Maintaining body temperature
- Providing proper nutrition (often via IV)
- Preventing infections
Complications of Respiratory Distress Syndrome
With timely treatment, many babies recover well. However, complications can occur, especially in severe cases.
Short-Term Complications
- Air leaks (pneumothorax)
- Infection (sepsis)
- Bleeding in the brain (intraventricular hemorrhage)
Long-Term Complications
- Bronchopulmonary dysplasia (BPD) – a chronic lung condition
- Developmental delays in some cases
- Increased risk of respiratory infections later in life
Babies requiring prolonged ventilator support are particularly at risk for BPD.
Respiratory Distress Syndrome in Adults (ARDS)
While neonatal RDS is due to immature lungs, Acute Respiratory Distress Syndrome (ARDS) in adults is caused by lung injury.
Common Causes of ARDS
- Severe infections (sepsis)
- Pneumonia
- Trauma or injury
- Inhalation of harmful substances
- Pancreatitis
Symptoms in Adults
- Severe shortness of breath
- Rapid breathing
- Low oxygen levels despite oxygen therapy
- Fatigue and confusion
ARDS is a medical emergency and requires intensive care.
Prevention of Respiratory Distress Syndrome
Prevention plays a key role, especially for high-risk pregnancies.
During Pregnancy
- Antenatal corticosteroids
Given to mothers at risk of preterm delivery to accelerate lung development - Proper diabetes management
Reduces risk in babies of diabetic mothers - Regular prenatal check-ups
Helps monitor fetal growth and development
At Birth
- Avoid unnecessary early C-sections
- Ensure delivery in a facility equipped with neonatal intensive care
Prognosis and Recovery
The outlook for babies with RDS has improved dramatically over the years due to advances in neonatal care.
What to Expect
- Mild cases recover within a few days
- Moderate cases may need support for a week or more
- Severe cases require intensive care but still have a good survival rate with modern treatment
Early intervention is the single biggest factor in improving outcomes.
Living with and Beyond Respiratory Distress Syndrome
For most infants, RDS is a temporary condition. However, follow-up care is essential.
Long-Term Care Includes
- Monitoring growth and development
- Regular pediatric check-ups
- Vaccinations to prevent respiratory infections
- Avoiding exposure to smoke and pollutants
Parents may feel anxious during recovery, but most babies go on to lead healthy lives.
When Should You Seek Medical Help?
Immediate medical attention is needed if a newborn shows:
- Difficulty breathing
- Persistent grunting or wheezing
- Bluish lips or skin
- Poor feeding or lethargy
For adults, symptoms like severe breathlessness and chest discomfort should never be ignored.
Frequently Asked Questions (FAQs)
1. What is the main cause of Respiratory Distress Syndrome?
The primary cause is a lack of surfactant in the lungs, especially in premature babies whose lungs are not fully developed.
2. Can full-term babies get RDS?
Yes, although it is less common. Factors like maternal diabetes or cesarean delivery can increase the risk even in full-term babies.
3. How is RDS different from ARDS?
- RDS (Neonatal): Caused by immature lungs and lack of surfactant
- ARDS (Adult): Caused by lung injury due to infection, trauma, or inflammation
4. Is Respiratory Distress Syndrome life-threatening?
It can be, especially in severe cases. However, with modern medical care, survival rates are high, particularly in specialized neonatal units.
5. How long does it take for a baby to recover from RDS?
Recovery can take anywhere from a few days to a few weeks, depending on severity and response to treatment.
6. Can RDS be prevented?
While not always preventable, the risk can be reduced with:
- Antenatal steroids
- Proper prenatal care
- Managing maternal health conditions
7. What is surfactant therapy?
It is a treatment where artificial surfactant is administered into the baby’s lungs to help keep air sacs open and improve breathing.
8. Are there long-term effects of RDS?
Most babies recover fully. However, some may develop chronic lung conditions like bronchopulmonary dysplasia.
9. Is mechanical ventilation always required?
No. Mild cases may only need oxygen or CPAP. Ventilation is used in more severe cases.
10. Can adults recover from ARDS?
Yes, but recovery may take time and often requires intensive care. Some individuals may experience long-term lung or physical weakness.
To consult a Pulmonologist at Sparsh Diagnostic Centre, call our helpline numbers 9830117733/ 8335049501.
#BhaloTheko
Disclaimer:
No content on this site, regardless of date, should ever be used as a substitute for direct medical advice from your doctor or other qualified clinician.

![]()