When your heart is working the way it should, blood flows in one direction—smoothly and efficiently. But in conditions like Aortic Regurgitation, that flow gets disrupted. Instead of moving forward, some of the blood leaks backward, forcing your heart to work harder than normal.
It may sound alarming—and in some cases, it is—but the good news is that with early detection and proper care, many people live full, active lives with this condition. Let’s break it down in a way that actually makes sense.
What Is Aortic Regurgitation?
Aortic regurgitation (AR) is a heart valve disorder where the aortic valve doesn’t close properly. This valve sits between the left ventricle (the heart’s main pumping chamber) and the aorta (the large artery carrying blood to the rest of your body).
When the valve fails to seal tightly, blood that should be moving forward leaks back into the left ventricle. Over time, this backflow increases the workload on the heart, causing it to enlarge and weaken.
Think of it like a faulty door that doesn’t shut completely—no matter how hard you push, some air (or in this case, blood) keeps slipping back through.
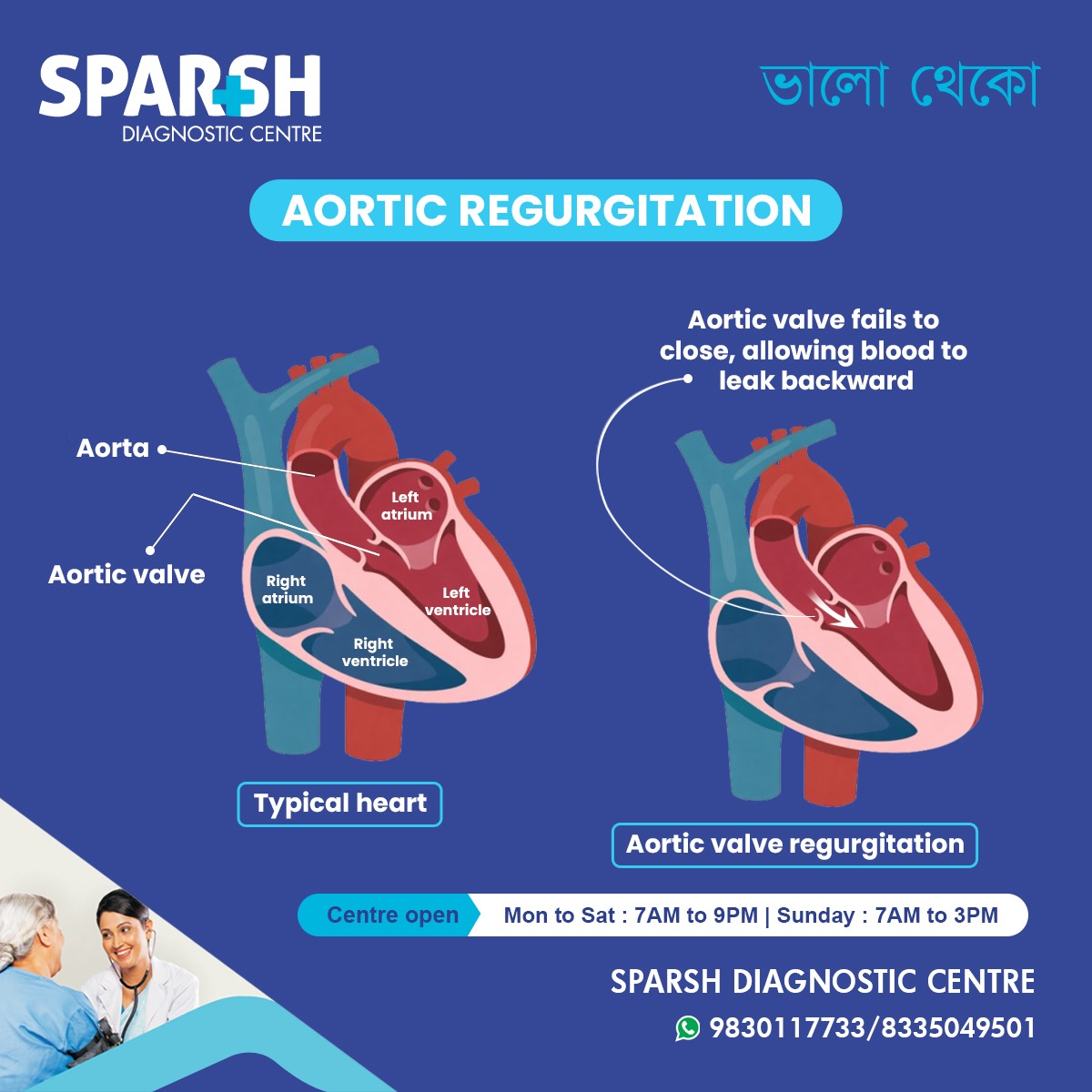
How the Heart Normally Works
To understand what goes wrong, it helps to know what “right” looks like.
- The left ventricle pumps oxygen-rich blood into the aorta.
- The aortic valve opens to let blood flow out.
- It then closes tightly to prevent blood from coming back.
In aortic regurgitation, that last step fails—allowing blood to leak backward into the heart.
Types of Aortic Regurgitation
Aortic regurgitation can develop in two main ways:
1. Acute Aortic Regurgitation
This comes on suddenly and is considered a medical emergency. It can be caused by:
- Infection of the valve
- Trauma or injury
- Sudden damage to the aorta
Symptoms appear quickly and can be severe.
2. Chronic Aortic Regurgitation
This develops slowly over years. The heart adapts at first, which is why many people don’t notice symptoms early on.
Over time, however, the heart struggles to keep up.
Causes of Aortic Regurgitation
There’s no single cause—AR can result from several underlying conditions:
Valve-Related Causes
- Congenital valve defects (like a bicuspid aortic valve)
- Age-related degeneration
- Calcification of the valve
Aortic Root Problems
- Enlargement of the aorta (aortic dilation)
- High blood pressure
- Connective tissue disorders (like Marfan syndrome)
Infections and Inflammation
Other Factors
- Chest trauma
- Autoimmune diseases
In many cases, especially in older adults, gradual wear and tear plays a major role.
Symptoms of Aortic Regurgitation
One tricky aspect of aortic regurgitation is that symptoms often don’t show up until the condition has progressed.
Early Stage (Often No Symptoms)
You may feel completely normal.
As It Progresses
You might notice:
- Shortness of breath, especially during activity
- Fatigue and weakness
- Heart palpitations (awareness of your heartbeat)
- Chest discomfort
- Lightheadedness or fainting
Advanced Symptoms
- Swelling in ankles and feet
- Difficulty breathing while lying down
- Rapid or irregular pulse
Because these symptoms overlap with other heart conditions, it’s easy to dismiss them. That’s why regular check-ups matter.
When Should You See a Doctor?
Don’t ignore symptoms like:
- Persistent shortness of breath
- Unusual fatigue
- Chest pain
- A pounding or irregular heartbeat
Even if they seem mild, they can signal underlying heart issues that need attention.
How Aortic Regurgitation Is Diagnosed
Diagnosis usually starts with a physical exam. A doctor may hear a characteristic heart murmur using a stethoscope.
From there, tests may include:
Echocardiogram
This is the most important test. It uses sound waves to create images of your heart and shows:
- Valve function
- Blood flow direction
- Heart size and strength
Electrocardiogram (ECG)
Checks your heart’s electrical activity.
Chest X-ray
Helps detect heart enlargement.
Cardiac MRI or CT Scan
Provides detailed images of the heart and aorta.
Stress Testing
Assesses how your heart performs during physical activity.
Complications of Aortic Regurgitation
If left untreated, AR can lead to serious problems:
- Heart failure
- Arrhythmias (irregular heart rhythms)
- Left ventricular enlargement
- Reduced heart function
The risk increases the longer the condition goes unmanaged.
Treatment Options
Treatment depends on how severe the condition is and whether symptoms are present.
1. Monitoring (Watchful Waiting)
If your condition is mild and you have no symptoms:
- Regular check-ups
- Periodic echocardiograms
- Lifestyle adjustments
2. Medications
While medications can’t fix the valve, they can reduce strain on the heart:
- Blood pressure medications
- Diuretics (to reduce fluid buildup)
- Vasodilators (to widen blood vessels)
3. Surgical Treatment
When the condition becomes severe, surgery may be necessary.
Aortic Valve Repair
In some cases, the existing valve can be repaired.
Aortic Valve Replacement
More commonly, the valve is replaced with:
- A mechanical valve (long-lasting but requires lifelong blood thinners)
- A biological valve (less durable but no long-term anticoagulation)
Surgery is typically recommended when:
- Symptoms appear
- Heart function declines
- The heart becomes enlarged
Lifestyle Tips for Managing Aortic Regurgitation
Living with AR doesn’t mean putting your life on hold. Small changes can make a big difference.
Stay Active (But Smart)
- Light to moderate exercise is usually safe
- Avoid overly strenuous activity unless cleared by your doctor
Monitor Your Blood Pressure
High blood pressure worsens the condition, so keep it under control.
Eat a Heart-Healthy Diet
Focus on:
- Fruits and vegetables
- Whole grains
- Lean protein
- Low sodium intake
Avoid Smoking and Excess Alcohol
Both can strain your heart.
Keep Up with Medical Appointments
Regular monitoring helps catch changes early.
Can Aortic Regurgitation Be Prevented?
Not always—but you can reduce your risk:
- Treat high blood pressure early
- Maintain good oral hygiene (to prevent infections like endocarditis)
- Manage chronic conditions
- Get regular health check-ups
Living with Aortic Regurgitation
Many people with mild or moderate AR live normal lives without major restrictions. The key is awareness and timely care.
If surgery is needed, outcomes today are excellent thanks to advancements in cardiac care.
The important thing is not to ignore symptoms or delay evaluation.
Frequently Asked Questions (FAQ)
1. Is aortic regurgitation life-threatening?
It can be if severe and untreated. However, with proper monitoring and timely treatment, most people manage it well.
2. Can aortic regurgitation go away on its own?
No. Once the valve is damaged, it doesn’t heal naturally. Treatment focuses on managing symptoms and preventing progression.
3. How fast does aortic regurgitation progress?
It varies. Some cases progress slowly over decades, while others worsen more quickly—especially if caused by infection or injury.
4. Can I exercise with aortic regurgitation?
Yes, in most cases. However, the type and intensity of exercise should be guided by your doctor.
5. Is surgery always required?
Not always. Surgery is only needed when the condition becomes severe or starts affecting heart function.
6. What happens if I ignore aortic regurgitation?
Ignoring it can lead to heart failure, arrhythmias, and other serious complications.
7. Are there warning signs before it becomes severe?
Yes—shortness of breath, fatigue, and palpitations are common early warning signs.
8. How long can you live with aortic regurgitation?
With proper care, many people live a normal lifespan, especially if treated at the right time.
To consult a Cardiologist at Sparsh Diagnostic Centre, call our helpline numbers 9830117733/ 8335049501.
#BhaloTheko
Disclaimer:
No content on this site, regardless of date, should ever be used as a substitute for direct medical advice from your doctor or other qualified clinician.

![]()





