If you’ve ever experienced sharp pain on the outside of your knee during a run, workout, or long walk, there’s a good chance you may be dealing with IT Band Syndrome. It’s one of the most common overuse injuries seen in runners, cyclists, and athletes who perform repetitive leg movements.
While the pain can feel frustrating and limiting, the good news is that IT Band Syndrome is usually treatable with the right combination of rest, stretching, strengthening exercises, and activity modification.
Understanding what causes the condition and how to manage it early can help prevent long-term discomfort and allow you to return to your normal activities safely.
What is the IT Band Syndrome?
IT Band Syndrome, also called Iliotibial Band Syndrome (ITBS), occurs when the iliotibial band becomes irritated or inflamed.
The iliotibial band, commonly known as the IT band, is a thick band of connective tissue that runs from the hip down the outside of the thigh and attaches near the knee. Its main role is to stabilize the knee and support movement during walking, running, and other activities.
When the IT band repeatedly rubs against the outer part of the knee, it can lead to inflammation and pain. This is why IT Band Syndrome is considered an overuse injury.
The condition most commonly affects:
- Runners
- Cyclists
- Hikers
- Football players
- Weightlifters
- People who suddenly increase physical activity
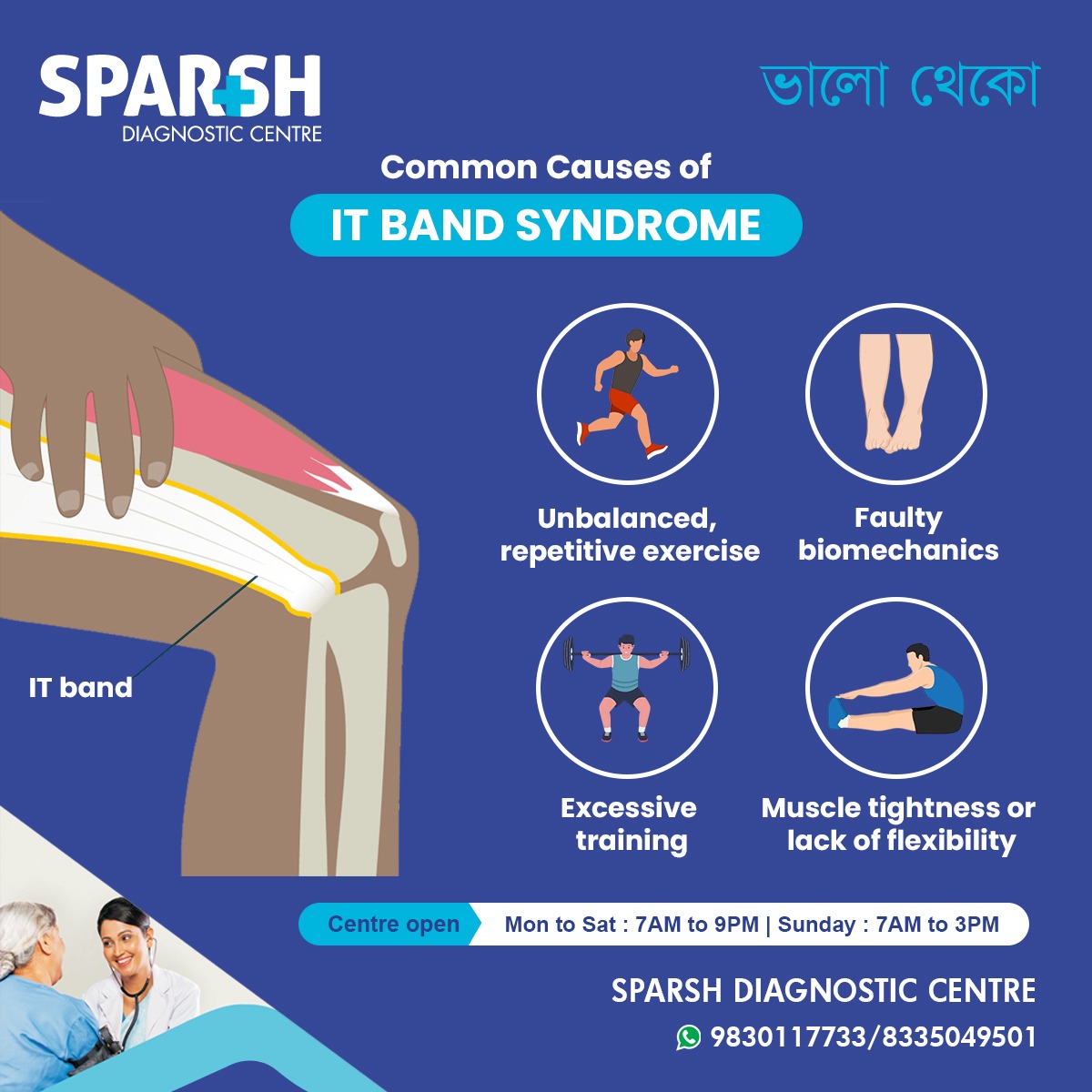
Causes of the IT Band Syndrome
IT Band Syndrome usually develops gradually rather than suddenly. It often happens because of repetitive stress on the knee and surrounding muscles.
Some of the most common causes include:
Repetitive Exercise
Running long distances, cycling for extended periods, or repetitive knee bending can strain the IT band over time.
Sudden Increase in Training
Increasing workout intensity, mileage, or duration too quickly can overload the muscles and connective tissues.
Muscle Tightness
Tight hip, thigh, or glute muscles can increase tension in the IT band, making irritation more likely.
Weak Hip Muscles
Weakness in the hip abductors and gluteal muscles can affect knee alignment and place additional stress on the IT band.
Poor Biomechanics
Issues such as flat feet, uneven leg length, improper running form, or abnormal gait patterns can contribute to the condition.
Inadequate Warm-Up
Skipping stretching or warm-up exercises before physical activity can increase injury risk.
Training on Uneven Surfaces
Running on sloped roads or uneven terrain may place extra strain on one side of the body.
Symptoms of IT Band Syndrome
The symptoms of IT Band Syndrome may start mildly and worsen over time if ignored.
Common symptoms include:
Pain on the Outside of the Knee
This is the hallmark symptom. The pain is usually sharp or burning and occurs on the outer side of the knee.
Pain During Activity
Discomfort often begins during running, cycling, climbing stairs, or prolonged walking.
Clicking or Snapping Sensation
Some individuals notice a snapping feeling around the knee when bending or straightening the leg.
Tenderness
The outer side of the knee may feel sore or sensitive to touch.
Tightness Along the Thigh
Tightness extending from the hip down the outer thigh is common.
Pain That Improves with Rest
Symptoms often decrease with rest but return once activity resumes.
Who Is at Risk for IT Band Syndrome?
Certain factors can increase the likelihood of developing IT Band Syndrome.
Athletes and Runners
Distance runners are especially vulnerable because of repetitive knee motion.
Cyclists
Improper bike setup or excessive cycling can contribute to irritation.
Beginners Starting Intense Workouts
People who suddenly begin high-intensity exercise programs may develop overuse injuries.
Individuals with Poor Flexibility
Limited flexibility in the hips and thighs increases tension in the IT band.
People with Biomechanical Issues
Flat feet, bowed legs, or poor posture can alter movement mechanics.
How is IT Band Syndrome diagnosed
Doctors typically diagnose IT Band Syndrome through a physical examination and medical history.
During the assessment, the healthcare provider may:
- Ask about symptoms and activity levels
- Examine the knee and hip
- Check flexibility and muscle strength
- Observe walking or running patterns
Specific movement tests may help identify IT band irritation.
Imaging tests such as X-rays or MRI scans are not always necessary but may be used to rule out other conditions like meniscus injuries or arthritis.
Treatment for IT Band Syndrome
Most cases improve with conservative treatment and lifestyle adjustments.
Rest and Activity Modification
Reducing or temporarily stopping aggravating activities is often the first step.
Avoid:
- Long-distance running
- Intense cycling
- Deep squats
- Repetitive knee bending
Switching to low-impact exercises like swimming may help maintain fitness during recovery.
Ice Therapy
Applying ice to the outer knee for 15–20 minutes several times daily can reduce pain and inflammation.
Anti-Inflammatory Medications
Over-the-counter medications may help manage discomfort. However, they should only be used under medical guidance.
Physical Therapy
Physical therapy is one of the most effective treatments for IT Band Syndrome.
A therapist may focus on:
- Stretching tight muscles
- Strengthening weak hip and glute muscles
- Improving flexibility
- Correcting movement patterns
- Teaching proper running mechanics
Foam Rolling
Foam rolling can help reduce tightness in the outer thigh and surrounding muscles.
Supportive Footwear
Wearing proper athletic shoes with adequate support can improve alignment and reduce strain.
Corticosteroid Injections
In severe cases, injections may help reduce inflammation temporarily.
Surgery
Surgery is rarely needed and is typically considered only after months of unsuccessful conservative treatment.
Best Exercises for IT Band Syndrome
Exercises play a major role in recovery and prevention.
IT Band Stretch
Stand upright and cross the affected leg behind the other. Lean sideways away from the painful side until you feel a stretch along the outer thigh.
Clamshell Exercise
Lie on your side with knees bent. Keeping feet together, lift the top knee while maintaining hip stability.
This exercise strengthens the glute muscles.
Side Leg Raises
Lifting the top leg while lying on your side helps strengthen hip stabilizers.
Glute Bridges
Lie on your back with knees bent and lift the hips upward while squeezing the glutes.
Foam Roller Stretch
Rolling the outer thigh gently over a foam roller may relieve tightness.
It’s important to perform exercises gradually and avoid movements that worsen pain.
Recovery Time for IT Band Syndrome
Recovery varies depending on severity and treatment consistency.
Mild cases may improve within a few weeks, while more severe cases can take several months.
Most people recover successfully when they:
- Rest adequately
- Follow rehabilitation exercises
- Correct training errors
- Avoid rushing back into activity
Returning to sports too early can increase the risk of recurrence.
How to Prevent IT Band Syndrome
Preventing IT Band Syndrome often involves improving training habits and body mechanics.
Increase Activity Gradually
Avoid sudden spikes in workout intensity or distance.
Warm Up Properly
Dynamic stretching and mobility exercises prepare the muscles for movement.
Strengthen Hip and Core Muscles
Strong stabilizing muscles help maintain proper alignment.
Stretch Regularly
Stretching the hips, hamstrings, and quadriceps can reduce tension.
Wear Proper Shoes
Replace worn-out footwear and choose shoes suited to your foot type.
Improve Running Technique
Proper posture and stride mechanics reduce stress on the knees.
Avoid Overtraining
Allow adequate recovery between workouts.
IT Band Syndrome in Runners
Runners are among the most affected groups because repetitive knee flexion increases friction around the IT band.
Common running-related risk factors include:
- Running downhill frequently
- Increasing mileage too quickly
- Poor running form
- Weak glute muscles
- Inadequate recovery
Many runners notice symptoms appearing after a certain distance into a run.
Early treatment is important because continuing to run through pain can worsen inflammation.
IT Band Syndrome vs Knee Injuries
IT Band Syndrome can sometimes be confused with other knee problems.
IT Band Syndrome
- Pain on the outer side of the knee
- Worse during repetitive movement
- Often linked to activity
Meniscus Injury
- May cause locking or catching
- Often follows twisting injury
- Pain deeper inside the knee
Patellofemoral Pain Syndrome
- Pain around the kneecap
- Worse when sitting for long periods
Knee Arthritis
- Stiffness and swelling
- More common in older adults
Proper diagnosis helps ensure the right treatment plan.
When to See a Doctor
Medical attention is recommended if:
- Knee pain persists despite rest
- Swelling becomes severe
- Walking becomes difficult
- Symptoms interfere with daily activities
- Pain keeps returning
Early evaluation can help prevent chronic problems.
Living with IT Band Syndrome
Recovering from IT Band Syndrome requires patience and consistency.
Many people feel tempted to push through pain, especially athletes and fitness enthusiasts. However, ignoring symptoms often prolongs recovery.
Listening to your body, following rehabilitation exercises, and making gradual adjustments to your activity routine can significantly improve outcomes.
Most individuals return to their normal activities successfully with proper care.
IT Band Syndrome is a common overuse injury that affects the outer knee and thigh. It frequently develops in runners, cyclists, and active individuals because of repetitive movement, muscle imbalances, or poor biomechanics.
Although the condition can be painful, most cases improve with conservative treatment such as rest, stretching, strengthening exercises, physical therapy, and proper training adjustments.
Recognizing symptoms early and addressing underlying causes are key to faster recovery and long-term prevention. With the right approach, most people can return to exercise safely and reduce the chances of the condition returning.
Frequently Asked Questions (FAQs)
What is the main cause of IT Band Syndrome?
The most common cause is repetitive knee movement combined with muscle tightness, overtraining, or poor biomechanics.
Where is IT Band pain located?
Pain is usually felt on the outer side of the knee and may extend along the outer thigh.
Can IT Band Syndrome heal on its own?
Mild cases may improve with rest and reduced activity, but proper stretching and strengthening are often needed for full recovery.
How long does IT Band Syndrome take to heal?
Recovery may take anywhere from a few weeks to several months depending on severity and treatment consistency.
Is walking good for IT Band Syndrome?
Gentle walking may be acceptable if it does not increase pain. However, high-impact activities should be limited during recovery.
Can stretching cure IT Band Syndrome?
Stretching helps reduce tightness, but strengthening exercises and correcting movement patterns are also important.
Is IT Band Syndrome serious?
It is usually not serious, but untreated cases can become chronic and interfere with physical activity.
Can cycling cause IT Band Syndrome?
Yes. Poor bike fit, excessive cycling, or repetitive knee bending can contribute to the condition.
Should I run with IT Band Syndrome?
Running through pain is not recommended because it may worsen inflammation and delay healing.
What exercises help IT Band Syndrome?
Clamshells, side leg raises, glute bridges, hip strengthening exercises, and IT band stretches are commonly recommended.
To consult an Orthopedic Surgeon at Sparsh Diagnostic Centre, call our helpline numbers 9830117733/ 8335049501.
#BhaloTheko
Disclaimer:
No content on this site, regardless of date, should ever be used as a substitute for direct medical advice from your doctor or other qualified clinician.

![]()