Knee pain can sneak into your life in the most frustrating ways—climbing stairs suddenly hurts, sitting too long becomes uncomfortable, or a simple jog feels like a challenge. One of the most common reasons behind this type of discomfort is Patellofemoral Pain Syndrome (PFPS), often referred to as “runner’s knee.”
Despite the nickname, you don’t have to be an athlete to experience it. PFPS affects people of all ages and activity levels, making it one of the leading causes of knee pain seen in clinics today.
Let’s break it down in a way that actually makes sense—what it is, why it happens, and how you can deal with it effectively.
What Is Patellofemoral Pain Syndrome?
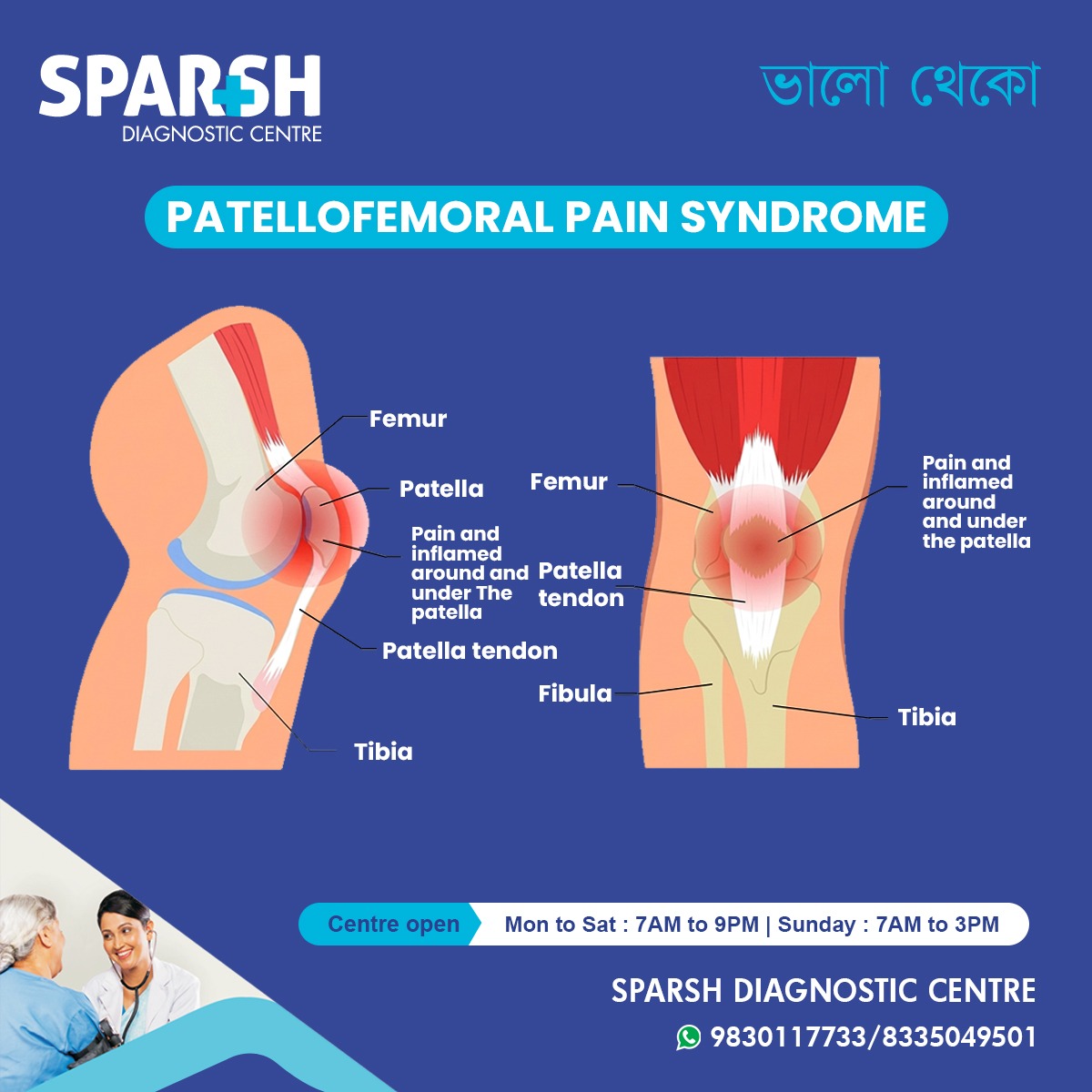
Patellofemoral Pain Syndrome is a condition characterized by pain around or behind the kneecap (patella). It occurs when the kneecap does not move smoothly over the groove of the thigh bone (femur) during movement.
In a healthy knee, the Patella glides seamlessly along the groove of the Femur. But when alignment or movement is off—even slightly—it creates stress on the joint, leading to irritation and pain.
This pain is typically felt:
- Around the front of the knee
- Behind the kneecap
- During movement or after prolonged sitting
Why Does It Happen?
PFPS doesn’t usually come from a single injury. Instead, it develops gradually due to multiple contributing factors.
1. Overuse and Repetitive Stress
Activities like running, squatting, jumping, or climbing stairs repeatedly put stress on the knee joint. Over time, this can irritate the tissues around the kneecap.
2. Poor Knee Alignment
If the kneecap doesn’t track properly in its groove, it leads to uneven pressure. This misalignment may be caused by:
- Flat feet
- Weak hip muscles
- Structural differences in the knee
3. Muscle Imbalance
The muscles around your knee and hip—especially the quadriceps—play a key role in stabilizing the patella. Weak or tight muscles can disrupt normal movement.
4. Injury or Trauma
A fall or direct blow to the knee can sometimes trigger PFPS.
5. Lifestyle Factors
Even non-athletes can develop PFPS due to:
- Prolonged sitting (common in desk jobs)
- Sudden increase in physical activity
- Wearing improper footwear
Common Symptoms to Watch For
PFPS symptoms are usually easy to recognize once you know what to look for.
Pain Patterns
- Dull, aching pain in the front of the knee
- Pain behind or around the kneecap
- Discomfort in one or both knees
Activity-Related Pain
You may feel pain when:
- Climbing or descending stairs
- Squatting or kneeling
- Running or walking long distances
- Sitting for long periods (often called “moviegoer’s knee”)
Other Signs
- A popping or grinding sensation in the knee
- Mild swelling around the kneecap
- Feeling of instability in the knee
Who Is at Risk?
While anyone can develop PFPS, certain groups are more prone:
- Athletes: Especially runners, cyclists, and football players
- Teenagers and young adults: Due to growth-related changes
- Women: Often due to wider hip structure affecting knee alignment
- People with sedentary lifestyles: Weak muscles can contribute to poor joint mechanics
How Is It Diagnosed?
Diagnosis of Patellofemoral Pain Syndrome is usually straightforward and doesn’t always require advanced testing.
Physical Examination
A doctor will:
- Check knee alignment
- Assess range of motion
- Evaluate muscle strength
- Look for tenderness around the patella
Imaging Tests (If Needed)
In some cases, doctors may recommend:
These tests help confirm the diagnosis and exclude other conditions like ligament injuries or arthritis.
Treatment Options That Actually Work
The good news? PFPS is highly treatable—and most people recover without surgery.
1. Rest and Activity Modification
Avoid activities that worsen the pain, especially high-impact exercises. This doesn’t mean complete inactivity—just smarter movement.
2. Ice Therapy
Applying ice packs for 15–20 minutes several times a day can reduce inflammation and pain.
3. Physiotherapy
This is the cornerstone of treatment. A structured exercise plan can:
- Strengthen quadriceps and hip muscles
- Improve kneecap alignment
- Restore normal movement patterns
4. Pain Relief Medication
Over-the-counter medications like Ibuprofen may help reduce pain and inflammation.
5. Knee Support
Braces or taping techniques can help guide the patella into proper alignment during movement.
6. Footwear and Orthotics
Supportive shoes or custom orthotics can correct foot mechanics, indirectly improving knee function.
Exercises That Help
Targeted exercises can significantly improve symptoms when done consistently.
Strengthening Exercises
- Straight leg raises
- Wall sits
- Step-ups
Stretching Exercises
- Hamstring stretches
- Calf stretches
- Quadriceps stretches
Hip Stability Work
- Clamshells
- Side leg raises
These exercises help stabilize the knee and reduce strain on the patella.
When Is Surgery Needed?
Surgery is rarely required for PFPS. It’s typically considered only if:
- Symptoms persist despite months of treatment
- There is significant structural misalignment
- Other knee conditions are present
Even in such cases, minimally invasive procedures are usually enough.
Recovery Timeline
Recovery varies depending on severity and adherence to treatment.
- Mild cases: 2–4 weeks
- Moderate cases: 1–3 months
- Chronic cases: 3–6 months or longer
Consistency with exercises and avoiding aggravating activities plays a huge role in recovery speed.
Prevention Tips That Make a Difference
Preventing PFPS is often easier than treating it.
Stay Active—but Smartly
Gradually increase intensity when starting new workouts.
Strengthen Supporting Muscles
Focus on hips, thighs, and core muscles.
Wear Proper Footwear
Choose shoes that offer good support and cushioning.
Maintain a Healthy Weight
Excess weight puts added pressure on the knees.
Avoid Prolonged Sitting
Take breaks to stretch and move around if you have a desk job.
When Should You See a Doctor?
You should seek medical advice if:
- Knee pain persists for more than a few weeks
- Pain worsens despite rest
- You experience swelling or instability
- Daily activities become difficult
Early diagnosis can prevent long-term complications.
Living with Patellofemoral Pain Syndrome
Managing PFPS is not just about treatment—it’s about adapting your lifestyle.
Small changes can make a big difference:
- Take stairs slowly instead of rushing
- Use proper posture while sitting
- Incorporate low-impact exercises like swimming or cycling
With the right approach, most people return to their normal activities without long-term issues.
FAQs About Patellofemoral Pain Syndrome
1. Is Patellofemoral Pain Syndrome serious?
Not usually. While it can be uncomfortable, it is rarely dangerous and responds well to treatment.
2. Can PFPS go away on its own?
Mild cases may improve with rest, but proper treatment speeds up recovery and prevents recurrence.
3. Is walking good for PFPS?
Yes, as long as it doesn’t cause pain. Low-impact activities are generally safe.
4. Can I run with PFPS?
It’s best to avoid running until pain improves. Gradual return is recommended under guidance.
5. Does PFPS affect both knees?
It can affect one or both knees, depending on underlying causes.
6. Are knee braces helpful?
Yes, they can provide support and improve alignment during movement.
7. How is PFPS different from arthritis?
PFPS is usually related to movement and alignment issues, while arthritis involves joint degeneration.
8. Can teenagers get PFPS?
Yes, especially during growth spurts when muscles and bones develop at different rates.
9. What is the fastest way to recover?
A combination of rest, physiotherapy, and strengthening exercises is the most effective approach.
10. Can PFPS come back?
Yes, if underlying issues like muscle weakness or poor mechanics are not addressed.
To consult an Orthopedic Surgeon at Sparsh Diagnostic Centre, call our helpline numbers 9830117733/ 8335049501.
#BhaloTheko
Disclaimer:
No content on this site, regardless of date, should ever be used as a substitute for direct medical advice from your doctor or other qualified clinician.

![]()