The first few moments after a baby is born are filled with emotion, relief, and a whirlwind of activity. While parents are soaking in that first cry, medical professionals are quickly assessing the newborn’s condition using something called the APGAR Score.
It’s a simple yet powerful test that gives doctors an immediate snapshot of how well your baby is adjusting to life outside the womb. If you’ve ever wondered what those numbers mean or why they matter, this guide breaks it all down in a clear, conversational way—no medical jargon overload.
What Is an APGAR Score?
The APGAR score is a quick evaluation performed on a newborn at 1 minute and 5 minutes after birth. In some cases, it may also be repeated at 10 minutes if needed.
The test was developed by Virginia Apgar in 1952 as a fast and reliable way to assess a baby’s physical condition and determine whether immediate medical care is required.
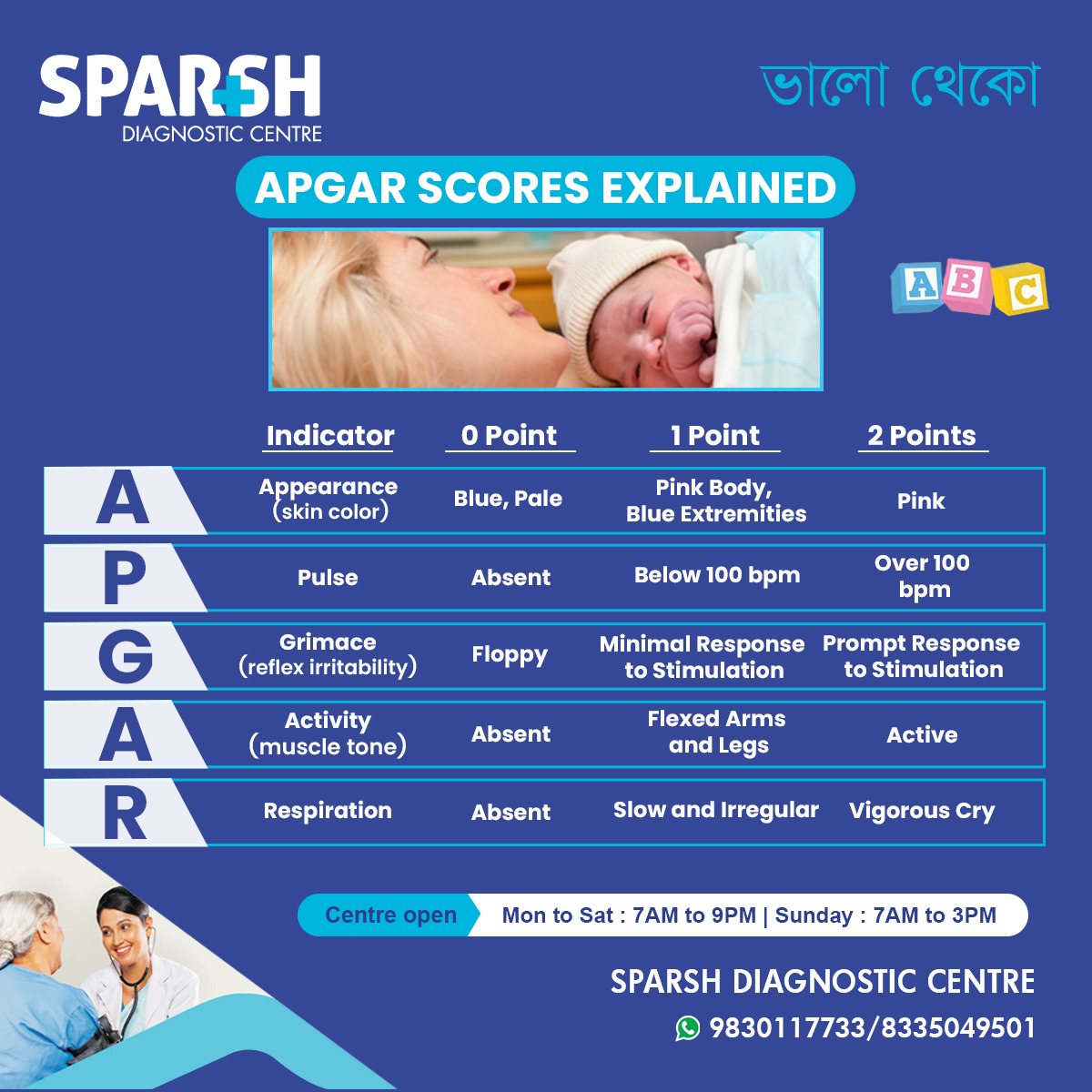
The name “APGAR” isn’t just a surname—it’s also a handy acronym:
- A – Appearance (skin color)
- P – Pulse (heart rate)
- G – Grimace (reflex response)
- A – Activity (muscle tone)
- R – Respiration (breathing effort)
Each of these five factors is scored on a scale of 0 to 2, with a maximum total score of 10.
Why Is the APGAR Score Important?
Here’s the thing: the APGAR score isn’t about predicting your baby’s future intelligence, health, or development. Instead, it’s a rapid assessment tool designed to answer one crucial question:
Does this baby need immediate medical support?
A low score doesn’t mean something is permanently wrong—it often just signals that the baby needs help adjusting, such as oxygen support or stimulation.
Think of it as a quick health check, not a long-term report card.
How the APGAR Score Is Calculated
Each of the five components is evaluated individually. Let’s take a closer look at what doctors are checking:
1. Appearance (Skin Color)
- 0 points: Blue or pale all over
- 1 point: Pink body with blue hands and feet
- 2 points: Completely pink
Skin color gives insight into how well oxygen is circulating in the baby’s body.
2. Pulse (Heart Rate)
- 0 points: No heartbeat
- 1 point: Fewer than 100 beats per minute
- 2 points: More than 100 beats per minute
Heart rate is one of the most critical indicators of a newborn’s stability.
3. Grimace (Reflex Irritability)
- 0 points: No response to stimulation
- 1 point: Minimal response (grimace)
- 2 points: Strong response like coughing, sneezing, or crying
This checks how well the baby responds to stimuli, such as a gentle pinch or suction.
4. Activity (Muscle Tone)
- 0 points: Limp and floppy
- 1 point: Some flexion of arms and legs
- 2 points: Active movement
Healthy babies usually show strong, spontaneous movement.
5. Respiration (Breathing Effort)
- 0 points: Not breathing
- 1 point: Weak or irregular breathing
- 2 points: Strong cry
A vigorous cry is often a reassuring sign that the lungs are working well.
Understanding APGAR Score Results
Once all five areas are scored, the numbers are added up to give a total between 0 and 10.
Here’s how those totals are typically interpreted:
7 to 10: Reassuring
Most babies fall into this range. It means the newborn is in good condition and usually doesn’t need special medical intervention.
4 to 6: Moderately Low
This suggests the baby may need some assistance—like oxygen, suctioning, or stimulation—to help stabilize.
0 to 3: Critically Low
A score in this range indicates the baby requires immediate medical attention, possibly including resuscitation.
Why Are Scores Taken Twice?
You might wonder why the APGAR score is measured at both 1 minute and 5 minutes.
- 1-minute score: Shows how well the baby tolerated the birth process
- 5-minute score: Indicates how well the baby is adapting to the new environment
If the 5-minute score is low, doctors may repeat the test every 5 minutes until the baby stabilizes.
What Affects an APGAR Score?
Several factors can influence a baby’s APGAR score, and not all of them are cause for concern.
Common Influences Include:
- Premature birth
- Difficult or prolonged labor
- Cesarean delivery
- Maternal medications during labor
- Birth complications
For example, premature babies often score lower initially because their bodies are still developing—not because something is “wrong.”
APGAR Score vs Long-Term Health
Let’s clear up a common misconception:
The APGAR score does NOT predict long-term health, intelligence, or development.
A baby with a low initial score can grow up perfectly healthy, while a baby with a high score still needs routine care and monitoring.
It’s simply a moment-in-time assessment.
What Happens If the Score Is Low?
If a newborn has a low APGAR score, medical staff act quickly. Depending on the situation, they may:
- Provide oxygen
- Clear the airway
- Stimulate breathing
- Use assisted ventilation
- Perform neonatal resuscitation if necessary
The goal is to stabilize the baby as quickly as possible. In many cases, babies respond well within minutes.
APGAR Scores in Premature Babies
Premature babies often have lower APGAR scores, especially at the 1-minute mark. This is because:
- Their lungs may not be fully developed
- Muscle tone may be weaker
- Reflex responses may be slower
Doctors take gestational age into account when interpreting these scores, so a slightly lower score isn’t automatically alarming.
Limitations of the APGAR Score
While the APGAR score is incredibly useful, it does have limitations:
- It doesn’t diagnose specific conditions
- It doesn’t predict neurological outcomes
- It can be influenced by temporary factors like medication or delivery method
That’s why doctors use it alongside other assessments rather than relying on it alone.
Why Parents Shouldn’t Panic About the Numbers
Hearing that your baby has a low APGAR score can be stressful—but context matters.
Many babies with low scores at 1 minute improve dramatically by 5 minutes. What matters most is how quickly the baby responds to care.
Doctors focus more on trends and response to treatment than a single number.
The Role of APGAR in Modern Neonatal Care
Even decades after its introduction, the APGAR score remains a cornerstone of newborn care worldwide. It’s quick, non-invasive, and provides immediate insight into a baby’s condition.
While modern medicine now includes advanced monitoring tools, the APGAR score continues to play a vital role in those critical first minutes of life.
Frequently Asked Questions (FAQ)
1. What is a normal APGAR score?
A score between 7 and 10 is considered normal and indicates that the baby is adapting well.
2. Should I worry if my baby has a low APGAR score?
Not necessarily. Many babies with low initial scores improve quickly with proper care. It’s not a predictor of long-term health.
3. Why is the APGAR score done at 1 and 5 minutes?
The first score assesses the baby’s condition immediately after birth, while the second shows how well they’re adjusting to life outside the womb.
4. Can a baby have a perfect APGAR score of 10?
Yes, but it’s relatively rare. Many healthy babies score 8 or 9 due to slightly bluish hands and feet right after birth.
5. Does a low APGAR score mean brain damage?
No. The APGAR score alone cannot diagnose brain damage or neurological conditions.
6. Do premature babies always have low APGAR scores?
They often have lower scores initially, but this is usually due to developmental immaturity rather than a serious problem.
7. Is the APGAR score painful for the baby?
No. It’s a quick observational assessment and involves minimal stimulation.
8. Who performs the APGAR test?
It’s usually done by a doctor, nurse, or midwife immediately after birth.
9. Can APGAR scores change over time?
Yes. That’s why multiple readings are taken. Scores often improve within minutes.
10. Is APGAR still used today?
Absolutely. Despite advances in neonatal care, it remains a standard and essential assessment tool worldwide.
The APGAR score is one of those medical tools that’s simple on the surface but incredibly valuable in practice. It gives healthcare providers a quick, structured way to ensure that newborns get the care they need right from the start.
For parents, understanding the APGAR score can ease anxiety and help you focus on what truly matters—your baby’s overall well-being, not just a number on a chart.
To consult a Pediatrician at Sparsh Diagnostic Centre, call our helpline numbers 9830117733/ 8335049501.
#BhaloTheko
Disclaimer:
No content on this site, regardless of date, should ever be used as a substitute for direct medical advice from your doctor or other qualified clinician.

![]()





